Blog
Items filtered by date: March 2026
Effective Blister Treatment for Faster Healing
Conservative and Advanced Care for Chronic Leg Wounds
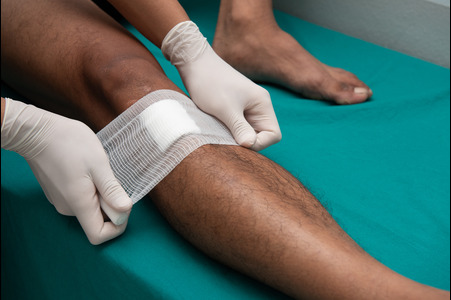
Chronic wounds on the legs often require layered care strategies that range from conservative measures to advanced therapies. Conservative treatment focuses on creating the best conditions for natural healing. This may involve cleaning the wound regularly, applying dressings that keep the environment balanced, relieving pressure with padding or footwear adjustments, and improving circulation through movement, leg elevation, or compression therapy, when appropriate. Nutrition, hydration, and managing underlying conditions such as diabetes or vascular disease are also critical to supporting recovery. When conservative methods are not enough, advanced treatments may be introduced. These can include debridement to remove non-healing tissue, cellular tissue products or skin substitutes to stimulate repair, and negative pressure wound therapy to draw out infection and promote closure. It is suggested that you see a wound care specialist to determine the right combination of treatments for your needs.
Chronic Wounds and Complications That Slow Recovery
Most wounds follow a predictable healing pattern, but some linger far longer than expected. Chronic wounds are those that fail to progress through normal healing, often remaining open, painful, and vulnerable to infection. On the feet, ankles, and legs, these stubborn wounds can significantly limit mobility and quality of life.
Post-surgical wounds are a common source of concern. While surgery is intended to improve health, the incision site does not always close as planned. Compromised circulation, infection, or pressure can delay healing and leave patients dealing with ongoing discomfort. Professional monitoring and care are essential to ensure the wound is cleaned, dressed, and supported until closure is achieved.
Chronic pain conditions may also complicate recovery. Neuromas, for example, are thickened nerve tissues that can cause persistent pain in the foot. Although not open wounds themselves, they often interfere with normal gait and create pressure points that make the skin more prone to breakdown. Left unaddressed, this discomfort can contribute to recurring sores or prevent existing wounds from closing.
Chronic wounds require specialized attention because traditional home remedies are rarely enough. Advanced wound care techniques may involve debridement, specialized dressings, pressure offloading, or therapies designed to improve blood flow and tissue repair.
If you have a wound on your foot, ankle, or leg that is not healing or continues to reopen, call us today for expert care from our wound specialist.
Understanding Pressure Ulcers on the Legs and Feet
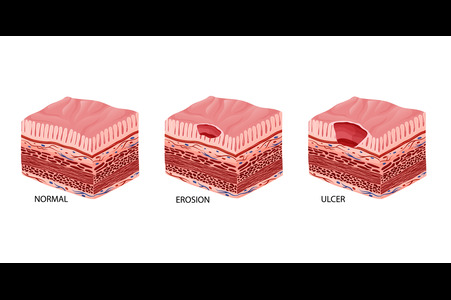
A pressure ulcer is a breakdown of skin and deeper tissue caused by prolonged force on one spot. On the legs, heels, and ankles, these wounds often form over bony areas where blood flow is easily reduced. When the skin does not receive enough oxygen and nutrients, it begins to weaken, eventually opening into a sore. Early signs include redness that does not fade, tenderness, warmth, or a spot that feels unusually firm or soft. If ignored, the ulcer can deepen and become difficult to heal, especially in people with diabetes, limited mobility, or circulation problems. These wounds can develop slowly and may go unnoticed at first, which is why regular skin checks are important. If you see ongoing redness, pain, or any open area on your legs or feet, it is suggested that you see a wound care specialist for proper evaluation and appropriate care.
Pressure Sores, Pressure Ulcers, and Arterial Ulcers Can Lead to Skin Breakdown
Not all wounds on the feet, ankles, and legs are the same. Pressure sores, pressure ulcers, and arterial ulcers may look similar at first, but develop for different reasons and require specialized care. Understanding these differences is key to proper treatment.
Pressure sores are often caused by friction at common rubbing points. Toes rubbing against each other can create small raw areas, while wearing ill-fitting shoes may lead to sores on the heel, ankle, or sides of the foot. These injuries usually begin at the surface but can quickly deepen if ignored.
Pressure ulcers, sometimes called bedsores, occur when the skin and tissue are compressed between bone and an external surface for long periods of time. On the lower extremities, they frequently appear on the heels, ankles, calves, or shins. Limited mobility, tight footwear, or prolonged bed rest can all contribute to these ulcers, which may progress through multiple stages from redness to open, infected wounds.
Arterial ulcers are different in that they result from poor circulation. When blood flow to the feet and legs is reduced, oxygen and nutrients cannot reach the tissue. Even small sores on the toes, heels, or shins may become painful, deep ulcers that heal very slowly. Unlike friction-related sores, arterial ulcers are directly tied to vascular health and often signal an underlying circulation problem.
All three types of wounds demand professional attention. A wound care specialist can determine the cause, relieve pressure, improve circulation when possible, and use advanced techniques to promote healing.
If you notice a sore on your foot, ankle, or leg that is slow to close or worsening, call us for timely care to help prevent serious complications and preserve long-term mobility.
Arterial Skin Ulcers on the Lower Legs and Feet
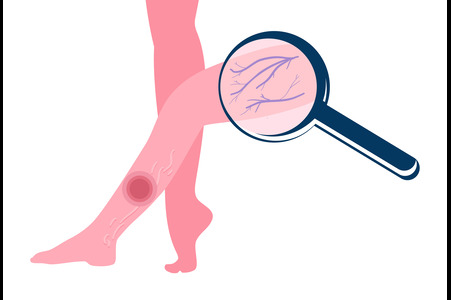
An arterial skin ulcer develops when poor blood flow prevents the skin and underlying tissues from receiving enough oxygen. These wounds often appear on the lower legs, tops of the feet, or toes, and are typically painful, especially at night or when the limb is elevated. The ulcer itself may look punched out with well-defined edges and a pale or dry wound bed. The surrounding skin can feel cool, look shiny, or show little hair growth due to reduced circulation. People with peripheral arterial disease, diabetes, or a history of smoking face a higher risk because their arteries are already compromised. These ulcers heal slowly without specialized care and may worsen if pressure or friction continues. Any persistent pain, discoloration, or open wound on the legs or feet should be evaluated promptly by a wound care specialist for an accurate diagnosis and treatment strategies.
Pressure Sores, Pressure Ulcers, and Arterial Ulcers Can Lead to Skin Breakdown
Not all wounds on the feet, ankles, and legs are the same. Pressure sores, pressure ulcers, and arterial ulcers may look similar at first, but develop for different reasons and require specialized care. Understanding these differences is key to proper treatment.
Pressure sores are often caused by friction at common rubbing points. Toes rubbing against each other can create small raw areas, while wearing ill-fitting shoes may lead to sores on the heel, ankle, or sides of the foot. These injuries usually begin at the surface but can quickly deepen if ignored.
Pressure ulcers, sometimes called bedsores, occur when the skin and tissue are compressed between bone and an external surface for long periods of time. On the lower extremities, they frequently appear on the heels, ankles, calves, or shins. Limited mobility, tight footwear, or prolonged bed rest can all contribute to these ulcers, which may progress through multiple stages from redness to open, infected wounds.
Arterial ulcers are different in that they result from poor circulation. When blood flow to the feet and legs is reduced, oxygen and nutrients cannot reach the tissue. Even small sores on the toes, heels, or shins may become painful, deep ulcers that heal very slowly. Unlike friction-related sores, arterial ulcers are directly tied to vascular health and often signal an underlying circulation problem.
All three types of wounds demand professional attention. A wound care specialist can determine the cause, relieve pressure, improve circulation when possible, and use advanced techniques to promote healing.
If you notice a sore on your foot, ankle, or leg that is slow to close or worsening, call us for timely care to help prevent serious complications and preserve long-term mobility.

